| 1-800-871-4350 |
 |
 |
 |
 |
 |
 |
 |
 |
 |
 |
| NARCONON FACTS |
|
Intervention is a process that helps an addict recognize the extent of his problem.
An important aspect of the Narconon program is the systematic application of techniques to improve communication and interpersonal skills in persons dependent on alcohol and/or drugs. Ignorance about or failure to abide by the common moral precepts of our society can lie at the root of many of the addict�s life problems. Narconon graduates are brought back to life, confident, in control and able to achieve their goals without the use of drugs. |
| RESOURCES |
 |
Ecstasy
MDMA was patented as long ago as 1913 by the German company Merck. Rumour has it that the drug was sold as a slimming pill along with comic descriptions of its strange side effects, although it was never marketed and the patent doesn't mention uses. The next time it came to light was in 1953 when the US army tested a number of drugs for military applications - again, folklore says it was tried as a truth drug but there is no evidence for this.(1)
The father of MDMA - or 'stepfather' as he describes himself - is Alexander Shulgin.(2) After obtaining a PhD in biochemistry from the University of California at Berkeley, Shulgin got a job as a research chemist with Dow Chemicals, for whom he invented a profitable insecticide. As a reward, the company gave him a free hand and his own lab. Having had an exciting experience on Mescaline, Shulgin used the opportunity to research psychedelic drugs. An accepted test for psychedelic effects was to observe how fighting fish change their behaviour. But there were problems: fish don't say when they are under the influence and, well, have you ever seen a fish that doesn't look stoned? His answer was to 'suck it and see'.
Eventually his company was embarrassed to find themselves holding the patents of some popular street drugs and he was politely given the push. Shulgin continued testing new compounds on himself and a select group of friends for many years. Thanks to his remarkable personality - combining openness without proselytising about his liberal and controversial views - he has earned the respect of influential people and is able to carry on with his research today, with the full approval of the US government. His approach to psychedelics is similar to that of a botanist: he specialises in the phenethylamines, and delights in recording the subtle differences between each member of that family of drugs. His experiences are described in his autobiography Phenethylamines I Have Known And Loved. MDMA is but one of 179 psychoactive drugs which he describes in detail, and, although its effects are less dramatic than many, MDMA is perhaps the one which comes closest to fulfilling his ambition of finding a therapeutic drug. Shulgin has now moved on to writing a book about another family of psychoactive drugs, the tryptamines, due out in 1995.
However, it was only after hearing glowing reports from other experimenters who had also synthesised and tried MDMA that Shulgin took an interest. He describes how in 1977 he gave some to an old friend who was about to retire from his career of psychotherapy.
He phoned me a few days later to tell me he had abandoned his plans for a quiet retirement. I know none of the details of the increasingly complex network which he proceeded to develop over the following decade, but I do know that he travelled across the country introducing MDMA to other therapists and teaching then how to use it in their therapy. They had all began, of course, by taking the drug themselves. He believed (as I do) that no therapist has the right to give a psychoactive drug to another person unless and until he is thoroughly familiar with its effects on his own mind. Many of the psychologists and psychiatrists whom Leo instructed developed small groups or enclaves of professionals who had been similarly taught, and the information and techniques he had introduced spread widely and, in time, internationally.
It is impossible to ever know the true breadth of therapeutic MDMA usage achieved during the remaining years of his life, but at his memorial service, I asked an old friend of his whether she had a guess at the number of people he had introduced to this incredible tool, either directly or indirectly. She was silent for a moment, then said, 'Well, I've thought about that, and I think probably around four thousand, give or take a few.' Those first psychotherapists to use MDMA were keenly aware that they had found a valuable new tool.(3, 4, 135) As one put it, "MDMA is penicillin for the soul, and you don't give up prescribing penicillin, once you've seen what it can do". They were equally aware that if MDMA became a popular street drug, it could follow in the footsteps of LSD and be criminalized by the US government. They agreed to do as much informal research as possible without bringing the drug to public attention, and did pretty well - MDMA only gradually became known as a fun drug and it wasn't until 1984 that the bubble burst.
If MDMA is so wonderful, why hasn't it been marketed by any of the big drug companies? One reason is that the drug's commercial potential is small; another was that the US Food and Drug Administration (FDA) prohibited trials on humans. But perhaps the most significant obstacle to the commercial exploitation of MDMA is that it has already been patented - although the patent ran out years ago, a drug cannot be patented a second time. Before marketing a new drug, a drug company has to show that the safety risks are justified by the drug's benefits as a medicine, and this involves long and expensive trials. The only way of recouping that expense is by obtaining exclusive rights to sell the drug through holding its patent.
Those years 1977 to 1985 are looked back on as the 'golden age' of Ecstasy or Adam(5) as it was then known. In psychotherapy, its use only appealed to a few experimental therapists since it didn't fit in with the usual 50-minute psychotherapy session, but they did include some of the most dynamic people in the field, including some who claimed that a five hour Adam session was as good as 5 months of therapy.(166) There was also a select a group of 'explorers' who used the drug in various ways, but, surprisingly, they never discovered its potential as a dance drug.
By 1984 the drug was still legal and was being used widely among students in the USA under its new name 'Ecstasy'. (Rumour has it that a big-time dealer called it 'Empathy', but, although the name is more appropriate, he found that Ecstasy had more sales appeal.) In Dallas and Fort Worth, Texas, Ecstasy was even on sale in bars where you could pay by credit card, where it replaced cocaine as the drug of choice among yuppies and even spread to people who normally kept well clear of drugs. However, it was this public and unashamed use that resulted in the drug being outlawed.
A deeply-embedded puritan ethic seems to affect the response to drugs in Western societies. To use a drug for pleasure is taboo(3), yet to use a drug to relieve pain is acceptable. In reality there is no sharp distinction: if someone is 'suffering from depression' and a drug makes him feel happy, it is regarded as a medicine and meets with approval. But if that person is regarded as normal and takes a drug that makes him happy, he is indulging in something quite unacceptable. Except, of course, if the drug happens to be nicotine or alcohol.(16)
During 1985 Ecstasy got into the mass media because a small group of people sued the US Drug Enforcement Agency to try to prevent them from outlawing the drug. The controversy provided free advertising which made Ecstasy spread like wildfire throughout the US. It was a case of bad timing - the previous year there had been a widely publicised disaster that made the authorities overreact to any new scare. A batch of 'China White', a so-called designer drug(6) which was sold to heroin addicts as a legal substitute, had contained a poisonous impurity, and, tragically, it caused a form of severe brain damage similar to Parkinson's disease.(7) As a result the US Congress passed a new law allowing the DEA to put an emergency ban on any drug it thought might be a danger to the public. On July 1st 1985 this right was used for the first time to ban MDMA - what is more, MDMA was put in the most restrictive category of all, reserved for damaging and addictive drugs without medical use.(8) The effect of prohibition was to curtail research into the drug without changing the attitudes of recreational users.(9) However, the Agency's haste was at the expense of not following the letter of the law, leaving the ruling to be overturned in subsequent court cases.
The temporary ban only lasted for a year; meanwhile a hearing was set up to decide what permanent measures should be taken against the drug. The case received much publicity and was accompanied by press reports advancing the kind of scare stories now current in Europe, which added to the pressure to make the ban permanent. One widely publicised report referred to evidence that another drug, MDA, caused brain damage in rats and concluded that MDMA could cause brain damage in humans.(10, 11, 12) The media indulged in horror scenarios of 'our kids' brains rotting by the time they were thirty, although there was no evidence that MDMA caused brain damage in rats at the dosage levels used by humans. On the other side were the psychotherapists who gave evidence of the benefits of the drug - but they had failed to prepare their ground by carrying out scientifically acceptable trials, so their evidence was regarded as 'anecdotal'.
The case ended with the judge recommending that MDMA be placed in a less restrictive category, Schedule 3, which would have allowed it to be manufactured, to be used on prescription and to be the subject of research. But the recommendation was ignored by the DEA, which refused to back down and instead placed MDMA permanently in Schedule 1. A group of MDMA supporters made a successful challenge to this decision in the Federal Court of Appeal, but their objections were overturned on 23rd March 1988. The fight is still continuing on the grounds that the law is unconstitutional, that the correct procedure was not followed and that the DEA did not take all the evidence into account.
In most countries including the US, all new drugs are regarded as 'innocent until proved guilty' unless they are substantially similar in structure and effect to prohibited drugs, and this gives rise to the phenomenon known as 'designer drugs' - drugs which have been deliberately synthesised to avoid the law. In Britain, however, whole families of chemicals - including members that have not been invented - are treated as 'guilty until proved innocent' under the law. Psychedelic amphetamines, which includes MDA, MDEA and MDMA have been illegal in Britain since 1977, and, as in the US, MDMA has been placed in the category that attracts highest penalties.(13, 14) All member countries of the United Nations are signatories to the International Convention on Psychotropic Substances (ICPO) and follow recommendations laid down by the World Health Organisation Expert Committee on Drug Dependence. In 1985, under American pressure, the ICPO asked member nations to place the drug in Schedule 1 although the chairman of the WHO Expert Committee disagreed with this decision, stating that "At this time, international control is not warranted." A clause was added encouraging member nations to "facilitate research on this interesting substance".(15)
The criminalisation of MDMA in America has had wide-ranging consequences. The first was to prevent the drug being used by professional therapists, except in Switzerland (see chapter 9). The second w as to reduce the quality of the drug as sold on the street, because demand was now met by clandestine laboratories and the drug was distributed through the criminal network. Although the number of users was dramatically reduced at first, criminalisation did not prevent the drug's popularity spreading worldwide.
Ecstasy
arrives in Europe
Ecstasy was favoured by Bhagwan Rajneesh, the Indian guru
whose disciples wore orange, and when his followers moved out of their ashram
in Oregon they brought the drug to Europe in the mid eighties.(17)
The rave scene started on the hippy holiday island of Ibiza in 1987, where Ecstasy joined LSD and hashish at all-night dance parties. In England 'raves' took the form of both large outdoor and warehouse parties, well described by Paul Staines in Appendix 3.
Warehouses were prepared secretly so as to avoid local people obtaining a court order to prevent the raves happening. Tickets were sold in advance without the address, but with a phone number to ring on the night for instructions regarding a meeting place such as a motorway service station from where a convoy would proceed to the venue. Opposition to raves was fierce since people living up to two miles away could be kept awake all night. By 1990 the British government had passed a law, the Entertainments (Increased Penalties Act)(18), which effectively put an end to these big gatherings.
The result was to push ravers into dance clubs. The Hacienda in Manchester led the trend in 1988 with the now prevalent style: DJs who never spoke, but teased the dancers with their subtle 'scratching' establishing the Manchester sound.(19) From there clubbing on E came to London, the rest of Europe and eventually back to E's native California, as reported in the San Francisco Examiner:
The English ravers hit San Francisco in the winter of 1991. "We were suddenly surrounded by these kids, moving here from England. They were coming here in droves and bringing with them a new sensibility, a new style of clothes."
By this time Ecstasy had reached nearly every corner of society in England and by the winter of 1991-2 demand had outstripped supply, partly due to some massive police seizures.(20, 21) Dealers responded by selling any old tablet as Ecstasy and no doubt made huge profits, but as a result people had disappointing experiences and turned away from Ecstasy. Many turned to LSD instead for the simple reason that the dose cannot be adulterated(13) as it is microscopic (a thousand times smaller than a dose of MDMA) and is normally sold absorbed into a 'blotter', a tiny piece of paper too small to absorb active quantities of any other popular drug.
The English pattern of use contrasts with the American one both in kind and volume, which accounts for there being so many more casualties here. The proportion of young people taking Ecstasy is many times higher in Britain(22, 23), and here it is nearly always used as a dance drug. Americans generally use Ecstasy at home, although English-style raves are on the increase.
Although the therapeutic use of MDMA has been outlawed in the US for the past seven years, steps are being taken there towards MDMA becoming a prescription drug. To comply with prerequisites for the licensing of new drugs, a non-profit organisation called The Multidisciplinary Association for Psychedelic Studies (MAPS) opened a Drug Master File for MDMA in 1986, thus permitting research into the drug to be conducted. Recently, research into the effects of MDMA in human volunteers has been approved by the FDA itself, and trials began in 1993.(24) I have faith in common sense prevailing over prejudice in the long run; unless new evidence emerges that MDMA is toxic or another drug appears that is even better, I believe that one day MDMA will be an acceptable medicine.
1.) Dominant Trend: Over the space of some three millennia, opium spread from its home in the eastern Mediterranean to China, creating an extended Asian opium zone. For the first time in recorded history, opium became a recreational drug in the cities of Mughal India.
2.) Implication: The persistent role of opiates as folk medicine and recreational euphoric for nearly 4,000 years raises questions about the chances of effecting its eradication in the near future.
b.) Early European Opium Trade (1640-1773):
1.) Dominant Trend: In this period, there was a shift from a limited trade in opium though intra-Asian networks to an expanding European commerce that stimulated both supply and demand. Working separately, European mercantile companies commercialized both opium cultivation and commerce, making it the basis of a profitable long distance trade in low-weight, high-value goods.
2.) Implication: During this era, opium's extraordinarily profitability, combining the constant demand of a staple with the high price of a luxury, becomes manifest. As an addictive drug, opium requires a daily dose giving it the inelastic demand of a basic foodstuff. Long distance sea-trade in bulk foods was still beyond the capacity of the era's maritime technology, but opium had the low weight and high mark-up of luxury goods like cloves or pepper. Compounding its profitability, the Chinese emperor prohibited opium in 1729, thus denying China the opportunity to produce opium and inadvertently conceding British merchants a de facto monopoly over the trade.
c.) European Mercantilism (1773-1858):
1.) Dominant Trend: Under the doctrine of mercantilism, all successful European colonial ventures in Asia involved commercialization of drugs in some form--caffeine, nicotine, or opiates. This 18th century trade transformed these drugs from luxury goods into commodities of mass consumption, making them integral to the economies and lifestyles of both Asian and Atlantic nations. Within the monopolistic logic of mercantilism, the British East India Company achieved the highest profits from its export of Indian opium to China because, from 1773 to 1830, its strong controls over key aspects--production, export, and sales.
2.) Implication: From the late 18th century onward, opium became a major trade commodity. Under the British East India Company (BEIC), centralized controls accelerated the export of Indian opium to China--from 13 tons in 1729 to and 2,558 tons in 1839.
d.) High Imperial Opium Trade (1858-1907):
1.) Dominant Trend: During the latter half of the 19th century, opium became a major global commodity. Across the Asian opium zone, from the Balkans to Manchuria, there was a steady increase of local opium cultivation and consumption. Moreover, in the latter half of the 19th century, the modern pharmaceutical industry made opiates a drug of mass abuse in the cities of the West--Europe, the Americas, and Australia.
2.) Implication: By the early 20th century, opium and its derivatives, morphine and heroin, had become a major global commodity equivalent in scale to other drugs such as coffee and tea.
e.) Multilateral Control (1907-1940):
1.) Dominant Trend: Within the Protestant churches of England and America a moral reaction to the excesses of a market-driven expansion of drug abuse inspired a global anti-opium movement in the late 19th Century. For the first time in the modern era, the anti-opium movement, in alliance with the larger temperance crusade, succeeded in winning new laws from the state restricting the individual's control over the body. With the passage of the Harrison Narcotics Act in 1914, the American state, for the first time, imposed the force of law over the right to use or abuse the body as the individual saw fit. Through a complex diplomacy from 1909 to 1925, the League of Nations adopted restrictions on the recreational use of heroin and opium that produced a major drop in legal production.
2.)
Implication: The prewar attempt at multilateral controls over narcotics had a
mixed result. Although repression did reduce both production and consumption,
the high profits inherent in the opiates traffic remained to sustain criminal
syndicates which now acted as an unintended market response to limit state control
over the drug trade.
Despite all these considerable drawbacks, multilateral
controls do have their successes. Through these efforts, the constant, century-long
upward trajectory in drug abuse was finally broken, and, for the first time since
the 18th century, both use and production began to decline. World opium production
dropped from 41,600 tons in 1907 to 16,600 tons in 1934, while licit world heroin
production fell sharply from an 20,000 lbs. in 1926 to only 2,200 lbs. in 1931.
f.) War & Transition (1940-1947):
1.) Dominant Trend: During World War II, restrictions on shipping and strict port security produced a marked hiatus in global opium trafficking. Denied illicit opiates from Asia, the United States drew limited supplies of low-grade heroin from Mexico that failed to meet even a fraction of consumer demand. By the end of the war, the US addict population had dropped to an historic low of some twenty thousand. Once smuggling resumed after the war, however, the US addict population resumed the habit.
2.) Implication: Under extreme circumstances, a reduction in drug supply can lead to a sudden, albeit ephemeral, decrease in consumption.
g.)
Cold War Opium Expansion (1948-1972):
1.)
Dominant Trend: The Cold War brought major changes to the world's illicit opium
traffic. The Communist victory in China eliminated the world's major opium market
within a decade, removing the globe's major producer and consumer of opiates from
the market. Although the Asian opium zone contracted geographically, Cold War
geo-politics, combined with illicit market forces, stimulated a steady increase
in opium production in the remaining area, which now stretched from Turkey to
Thailand.
Supplied by the Asian zone, other markets--particularly in the United
States and Iran--expanded their consumption of opiates steadily during this period.
2.) Implication: External intervention in the remote tribal areas along the Asian opium zone contributed to the rise of drug lords and their armies, allowing them to position themselves for a massive expansion of local opium production. By providing arms, logistics, organization, and political protection, external alliances created the preconditions for a later leap in opium production in Burma and Afghanistan.
h.) US Bilateral Suppression (1973-1979):
1.) Dominant Trend: Although repression disrupted the global heroin trade for several years, over the longer term Nixon's drug war stimulated both opium production and heroin consumption. Ignoring these lessons, the Reagan and Bush administrations later pursued parallel policies in Latin America with dismal results. In essence, all three drug wars extended a local law enforcement model into the international arena in a way that failed to reduce either drug production or exports. Stimulated in part by three US drug wars, Asian opium production increased from 1,000 tons in 1970 to 4,000 tons in 1989.
2.)
Implication: When law enforcement is applied to such an elaborate commerce, drug
syndicates usually react in ways not foreseen by enforcement agencies. Treating
this global commodity trade as if it were a localized vice, U.S. drug agencies
often apply repression without any awareness of the intricate dynamics of these
worldwide marketing systems. For both legal and illicit commodities, a crop failure
in one production zone--whether from war, drought, or disease--creates a shortage
of supply and raises the price for producers elsewhere, stimulating increased
production in the next crop cycle.
i.) Increase in Asian Zone (1979-1989):
1.) Dominant Trend: For the first time in opium's history, highland drug lords began to act as independent entrepreneurs, responding creatively to market opportunities for their product. In Burma, for example, opium production increased exponentially from 550 tons in 1981 to 2,500 in 1989, in large part through the efforts of leading warlords like Khun Sa. Similarly, the emergence of Gulbuddin Hekmatyar as the dominant rebel leader in Afghanistan created a parallel figure of power who could control much of the country's opium production, heroin processing, and export.
2.) Implication: The capacity of powerful opium warlords in Burma and Afghanistan to both produce and export has had a growing influence on Western heroin markets--sending vast new supplies of Burmese heroin to America and giving the Sicilian mafia a major new role as brokers for South West Asian heroin to Europe and the United States.
j.) Global Proliferation of Opium (1989-1994):
1.) Dominant Trend: In the early 1990s, heroin recovered its historic preeminence as a leading illicit narcotic and became something of a "world" drug. Expansion of established opium areas in Burma and Afghanistan, combined with introduction of the crop into Central Asia and Latin America, led to a steady increase in world supply. Increased opium harvests have led to a dramatic proliferation of heroin abuse around the globe--a phenomenon so vast that we can speak, without hyperbole, of a "globalization" of heroin consumption. Paralleling the rise of use in established consuming regions, heroin abuse shot upward in new areas of Europe and Asia.
2.) Implication: World opium supply is growing without any apparent restraint. Since all opium produced is always consumed, rising supply is now a powerful force driving a sharp increase in world heroin consumption, creating insatiable demand for the drug, not seen since early 19th Century China, that may, in turn, yield further production increases in Latin America or Central Asia.
History of Marijuana & Cannabis Timeline
courtesy erowid.org
6000
B.C. Cannabis seeds used for food in China
4000 B.C. Textiles made of
hemp are used in China. (Pharmacotheon)
2727 B.C. First recorded use of
cannabis as medicine in Chinese pharmacopoeia. In every part of the world humankind
has used cannabis for a wide variety of health problems.
1500 B.C. Cannabis
cultivated in China for food and fiber
1500 B.C. Scythians cultivate cannabis
and use it to weave fine hemp cloth. (Sumach 1975)
1200-800 B.C. Cannabis
is mentioned in the Hindu sacred text Atharvaveda (Science of Charms) as "Sacred
Grass", one of the five sacred plants of India. It is used by medicinally
and ritually as an offering to Shiva.
700-600 B.C. The Zoroastrian Zend-Avesta,
an ancient Persian religious text of several hundred volumes, and said to have
been written by Zarathustra (Zoroaster), refers to bhang as Zoroaster's "good
narcotic" (Vendidad or The Law Against Demons)
700-300 B.C. Scythian
tribes leave Cannabis seeds as offerings in royal tombs.
500 B.C. Scythian
couple die and are buried with two small tents covering censers. Attached to one
tent stick was a decorated leather pouch containing wild Cannabis seeds. This
closely matches the stories told by Herodotus. The gravesite, discovered in the
late 1940s, was in Pazryk, northwest of the Tien Shan Mountains in modern-day
Khazakstan.
500 B.C. Hemp is introduced into Northern Europe by the Scythians.
An urn containing leaves and seeds of the Cannabis plant, unearthed near Berlin,
is dated to about this time.
500-100 B.C. Hemp spreads throughout northern
Europe.
430 B.C. Herodotus reports on both ritual and recreation use of
Cannabis by the Scythians (Herodotus The Histories 430 B.C. trans. G. Rawlinson).
100 B.C.-0 The psychotropic properties of Cannabis are mentioned in the
newly compiled herbal Pen Ts'ao Ching which is attributed to an emperor c. 2700
B.C.
0-100 A.D. Construction of Samartian gold and glass paste stash box
for storing hashish, coriander, or salt, buried in Siberian tomb.
70 A.D.
Dioscorides mentions the use of Cannabis as a Roman medicament.
170 A.D.
Galen (Roman) alludes to the psychoactivity of Cannabis seed confections.
500-600
A.D. The Jewish Talmud mentions the euphoriant properties of Cannabis. (Abel 1980)
900-1000 A.D. Scholars debate the pros and cons of eating hashish. Use
spreads throughout Arabia.
1090-1256 A.D. In Khorasan, Persia, Hasan ibn
al-Sabbah, the Old Man of the Mountain, recruits followers to commit assassinations...legends
develop around their supposed use of hashish. These legends are some of the earliest
written tales of the discovery of the inebriating powers of Cannabis and the supposed
use of Hashish. 1256 Alamut falls
1200s Cannabis is introduced in Egypt
during the reign of the Ayyubid dynasty on the occasion of the flooding of Egypt
by mystic devotees coming from Syria. (M.K. Hussein 1957 - Soueif 1972)
Early
1200s Hashish smoking very popular throughout the Middle East.
1155-1221
Persian legend of the Sufi master Sheik Haidar's of Khorasan's personal discovery
of Cannabis and it's subsequent spread to Iraq, Bahrain, Egypt and Syria. Another
of the ealiest written narratives of the use of Cannabis as an inebriant.
1300s
The oldest monograph on hashish, Zahr al-'arish fi tahrim al-hashish, was written.
It has since been lost.
1300s Ibn al-Baytar of Spain provides a description
of psychaoctive Cannabis.
1300s Arab traders bring Cannabis to the Mozambique
coast of Africa.
1231 Hashish introduced to Iraq in the reign of Caliph
Mustansir (Rosenthal 1971)
1271-1295 Journeys of Marco Polo in which he
gives second-hand reports of the story of Hasan ibn al-Sabbah and his "assassins"
using hashish. First time reports of Cannabis have been brought to the attention
of Europe.
1378 Ottoman Emir Soudoun Scheikhouni issues one of the first
edicts against the eating of hashish.
1526 Babur Nama, first emperor and
founder of Mughal Empire learned of hashish in Afghanistan.
mid 1600s
The epic poem, Benk u Bode, by the poet Mohammed Ebn Soleiman Foruli of Baghdad,
deals allegorically with a dialectical battle between wine and hashish.
1700s
Use of hashish, alcohol, and opium spreads among the population of occupied Constantinople
Late 1700s Hashish becomes a major trade item between Central Asia and
South Asia.
1798 Napoleon discovers that much of the Egyptian lower class
habitually uses hashish (Kimmens 1977). He declares a total prohibition. Soldiers
returning to France bring the tradition with them.
1900s Hashish production
expands from Russian Turkestan into Yarkand in Chinese Turkestan.
1809
Antoine Sylvestre de Sacy, a leading Arabist, reveals the etymology of the words
"assassin" and "hashishin"
1840 In America, medicinal
preparations with a Cannabis base are available. Hashish available in Persian
pharmacies.
1843 Le Club des Hachichins, or Hashish Eater's Club, established
in Paris.
after 1850 Hashish appears in Greece.
1856 British tax ganja
and charas trade in India
1870-1880 First reports of hashish smoking on
Greek mainland
c. 1875 Cultivation for hashish introduced to Greece
1877
Kerr reports on Indian ganja and charas trade.
1890 Greek Department of
Interior prohibits importance, cultivation and use of hashish.
1890 Hashish
made illegal in Turkey
1893-1894 The India Hemp Drugs Commission Report
is issued.
1893-1894 70,000 to 80,000 kg of hashish legally imported into
India from Central Asia each year.
Early 2000s Hashish smoking very popular
throughout the Middle East.
1915-1927 Cannabis begins to be prohibited
for nonmedical use in the U.S., especially in SW states...California (1915), Texas
(1919), Louisiana (1924), and New York (1927).
1920 Metaxus dictators
in Greece crack down on hashish smoking.
1920s Hashish smuggled into Egypt
from Greece, Syria, Lebanon, Turkey, and Central Asia
1926 Lebanese hashish
production peaks after World War I until prohibited in 1926.
1928 Recrational
use of Cannabis is banned in Britain.
1920s-1930s High-quality hashish
produced in Turkey near Greek border.
1930 Yarkand region of Chinese Turkestan
exports 91,471 kg of hashish legally into the Northwest Frontier and Punjab regions
of India
1930s Legal taxed imports of hashish continue into India from
Central Asia.
1934-1935 Chinese government moves to end all Cannabis cultivation
in Yarkand and charas traffic from Yarkand. Both licit and illicit hashish production
become illegal in Chinese Turkestan.
1937 Cannabis made federally illegal
in the U.S. with the passage of the Marihuana Tax Act.
1938 Supply of
hashish from chinese Turkestan nearly ceases.
1940s Greek hashish smoking
tradition fades.
1941 Indian government considers cultivation in Kashmir
to fill void of hashish from Chinese Turkestan.
1941-1942 Hand-rubbed
charas from Nepal is choicest hashish in India during World War II.
1945
Legal hashish consumption continues in India
1945-1955 Hashish use in
Greece flourishes again
1950s Hashish still smuggled into India from Chinese
Central Asia
1950s Moroccan government tacitly allows kif cultivation
in Rif Mountains.
1962 First hashish made in Morocco.
1963 Turkish
police seize 2.5 tons of hashish
1965 First reports of C. afghanica use
for hashish production in northern Afghanistan
1965 Mustafa comes to Ketama
in Morocco to make hashish from local kif.
1966 The Moroccan government
attempts to purge kif growers from Rif Mountains.
1967 "Smash",
the first hashish oil appears. Red Lebanese reaches California.
Late 1960s-Early
1970s The Brotherhood popularizes Afghani hashish.
1970-1973 Huge fields
of Cannabis cultivated for hashish production in Afghanistan. Last years that
truly great afghani hashish is available
Oct 27, 1970 The Comprehensive
Drug Abuse Prevention and Control Act is passed. Part II of this is the Controlled
Substance Act (CSA) which defines a scheduling system for drugs and places most
of the known hallucinogens (LSD, psilocybin, psilocin, mescaline, peyote, cannabis)
in Schedule I.
1972 The Nixon-appointed Shafer Commission urged use of
cannabis be re-legalized, but their recommendation was ignored. Medical research
continues. 1
Early 1970s Lebanese red and blonde hashish of very high-quality
exported. The highest quality Turkish hashish from Gaziantep near Syria appears
in western Europe.
Early 1970s Afghani hashish varieties introduced to
North America for sinsemilla production. Westerners bring metal sieve cloths to
Afghanistan. Law enforcement efforts against hashish begin in Afghanistan
1973
Nepal bans the Cannabis shops and charas (hand-rolled hash) export.
1973
Afghan government makes hashish production and sales illegal. Afghani harvest
is pitifully small.
1975 FDA establishes Compassionate Use program for
medical marijuana.
1976-1977 Quality of Lebanese hashish reaches zenith.
1978 Westerners make sieved hashish in Nepal from wild Cannabis.
Late
1970s Increasing manufacture of "modern" Afghani hashish. Cannabis varieties
from Afghanistan imported into Kashmir for sieved hashish production.
1980s
Morocco becomes one of, if not the largest, hashish producing and exporting nations.
1980s "Border" hashish produced in northwestern Pakistan along
the Afghan border to avoid Soviet-Afghan war.
1985 Hashish still produced
by Muslims of Kashgar and Yarkland (NW China).
1986 Most private stashes
of pre-war Afghani hashish in Amsterdam, Goa, and America are nearly finished.
1987 Moroccan government cracks down upon Cannabis cultivation in lower
eleations of Rif Mountains.
1988 DEA administrative law Judge Francis
Young finds after thorough hearings that marijuana has clearly established medical
use and should be reclassified as a prescriptive drug.
1993 Cannabis eradication
efforts resume in Morocco.
1994 Heavy fighting between rival Muslim clans
continues to upset hashish trade in Afghanistan
1994 Border hashish still
produced in Pakistan.
1995 Introduction of hashish-making equipment and
appearance of locally produced hashish in Amsterdam coffee shops.
Early methamphetamine
First
synthesized in 1887 Germany, amphetamine was for a long time, a drug in search
of a disease. Nothing was done with the drug, from its discovery (synthesis) until
the late 1920's, when it was seriously investigated as a cure or treatement against
nearly everything from depression to decongestion.
In the 1930's, amphetamine was marketed as Benzedrine in an over-the-counter inhaler to treat nasal congestion (for asthmatics, hay fever sufferers, and people with colds). A probable direct reaction to the Depression and Prohibition, the drug was used and abused by non-asthmatics looking for a buzz. By 1937 amphetamine was available by prescription in tablet form.
Methamphetamine, more potent and easy to make, was discovered in Japan in 1919. The crystalline powder was soluble in water, making it a perfect candidate for injection. It is still legally produced in the U.S., sold under the trade name Desoxyn.
During World War II, amphetamines were widely used to keep the fighting men going (during the Viet Nam war, American soldiers used more amphetamines than the rest of the world did during WWII). In Japan, intravenous methamphetamine abuse reached epidemic proportions immediately after World War II, when supplies stored for military use became available to the public.
In the United States in the 1950s, legally manufactured tablets of both dextroamphetamine (Dexedrine) and methamphetamine (Methedrine) became readily available and were used non medically by college students, truck drivers, and athletes, As use of amphetamines spread, so did their abuse. Amphetamines became a cure-all for such things as weight control to treating mild depression.
This pattern changed drastically in the 1960s with the increased availability of injectable methamphetamine. The 1970 Controlled Substances Act severely restricted the legal production of injectable methamphetamine, causing its use to decrease greatly.
Methamphetamine trafficking and abuse in the United States have been on the rise over the past few years, as indicated by investigative, seizure, price, purity, and abuse data (see "trends" below). As a result, this drug is having a devastating impact in many communities across the nation. Although more common in western areas of the country, this impact increasingly is being felt in areas not previously familiar with the harmful effects of this powerful stimulant.
Clandestine production accounts for almost all of the methamphetamine trafficked and abused in the United States. The illicit manufacture of methamphetamine can be accomplished in a variety of ways, but is produced most commonly using the ephedrine/pseudoephedrine reduction method. Large-scale production of methamphetamine using this method is dependent on ready access to bulk quantities of ephedrine and pseudoephedrine. During the past two years, several bulk ephedrine seizures destined for Mexico focused attention on the magnitude of ephedrine acquisition by organized crime drug groups operating from Mexico and in the United States, and set in motion an effort to focus international attention on the ephedrine diversion problem and to take action to prevent such diversion.
Drug law enforcement efforts against clandestine methamphetamine producers constitute a "cat and mouse" game between efforts to cut off chemical supplies and efforts to obtain them from non-regulated sources. Past experience has demonstrated that methamphetamine traffickers are relentless, flexible, and creative in finding new ways to obtain chemicals by evading the network of international controls that has been established. The Federal Government currently is preparing regulations to further reduce the diversion of pharmaceutical products containing chemicals, such as ephedrine and pseudoephedrine, that can be used to produce illegal drugs. It has consulted with corporations within the pharmaceutical industry to develop a solution to the diversion problem that does not unduly restrict the availability of these chemicals for legitimate use.
Domestically, large-scale production of methamphetamine is centered in California. In addition, methamphetamine increasingly is produced in Mexico and smuggled into the United States. Methamphetamine laboratory operators often are well-armed, and their laboratories occasionally are booby-trapped and equipped with scanning devices employed as security precautions. Weaponry, ranging from single firearms to arsenals of high-powered weapons and explosives, are commonly found at laboratory sites. Not only are methamphetamine laboratories used to manufacture illegal, often deadly drugs, but the clandestine nature of the manufacturing process and the presence of ignitable, corrosive, reactive, and toxic chemicals at the sites have resulted in explosions, fires, toxic fumes, and irreparable damage to human health and to the environment.
Traditionally, the suppliers of methamphetamine throughout the United States have been outlaw motorcycle gangs and numerous other independent trafficking groups. Although these groups continue to produce and distribute methamphetamine, organized crime drug groups operating from Mexico currently dominate wholesale methamphetamine trafficking in the United States for several reasons: these organizations established access to wholesale ephedrine sources of supply on the international market; these organizations are producing unprecedented quantities of high-purity methamphetamine on a regular basis; and, they already control well-established cocaine, heroin, and marijuana distribution networks throughout the western United States, enabling them to supply methamphetamine to a large retail level market. Their expansion into the methamphetamine trade has added a new dimension to their role in the U.S. drug market and has redefined the methamphetamine problem in the United States. Presently, these organizations are poised to supply methamphetamine to the rest of the country in response to any increases in demand.
Trends in methamphetamine use
As we begin 1997, the West, Southwest, and the South there are reports of methamphetamine and ephedrine as emerging drugs. According to DEA sources, Mexican manufacturers and distributors have replaced the outlaw motorcycle groups which had produced methamphetamine supplies for over twenty years. The new manufacturers are producing large quantities of high purity methamphetamine on both sides of the border, drawing on the legal supply of the precursor chemicals on the Mexican side. The price of methamphetamine had dropped significantly (to approximately $3000/pound in Southern California) until recent efforts to curtail ephedrine/pseudoephedrine supplies produced a slight shortage in some areas and a corresponding price increase. In Washington State, sources report that the resultant price increase has caused a number of methamphetamine users in that area to switch to cocaine.
One Texas source cited a number of reports of adverse effects of ephedrine and pseudoephedrine, a common substance in a number of over the counter and/or health food products. Ephedrine tablets can be purchased in Mexico and are often seized at the border or in other locations in transit to U.S.-based manufacturers. Some of the ephedrine/pseudoephedrine products readily available in Texas include 40 or 50 milligrams of ephedrine as well as substantial quantities of caffeine. Adverse consequences of their use include agitation, palpitations, and fainting from the stimulant effect. Called "herbal ecstasy" in both Texas and Southern California and touted as "safe" or "legal" MDMA, it is reportedly available from some health food stores or through mail order.
Methamphetamine continues to be popular in San Francisco. The ethnographer from that area reports that in addition to its use by young users who combine it with heroin ("a meth speedball") it can also be found in "biker's coffee," a combination of methamphetamine and coffee popular among young, fairly affluent urbanites. This is similar to the population of users described by the Los Angeles source. In that area, users are primarily snorting methamphetamine rather than smoking it as "ice" or injecting it.
Methamphetamine: A Dangerous Drug, A Spreading Threat
Methamphetamine is a highly addictive drug that can be manufactured by using products commercially available anywhere in the United States. The chemicals used in producing methamphetamine are extremely volatile, and the amateur chemists running makeshift laboratories -- often in hotels or areas where children are present -- cause deadly explosions and fires. The by-products of methamphetamine production are extremely toxic. Methamphetamine traffickers display no concern about environmental hazards when it comes to manufacturing and disposing of methamphetamine and its by-products.
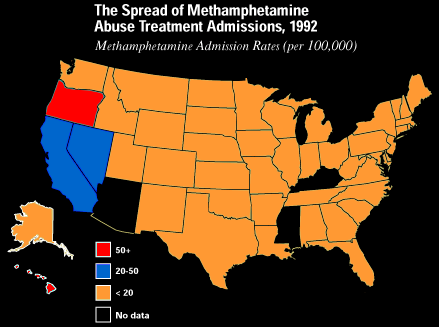
The effects of methamphetamine on humans are profound. SAMHSA is currently testing the effectiveness of various treatment regimens for methamphetamine, an addiction that is extremely difficult to treat. The stimulant effects from methamphetamine can last for hours, instead of minutes as with crack cocaine. Often the methamphetamine user remains awake for days. As the high begins to wear off, the methamphetamine user enters a stage called "tweaking," in which he or she is prone to violence, delusions, and paranoia. Many methamphetamine users try to alleviate the effect of the methamphetamine "crash" by buffering the effects with other drugs such as cocaine or heroin. Like heroin and cocaine, methamphetamine can be snorted,smoked, or injected.
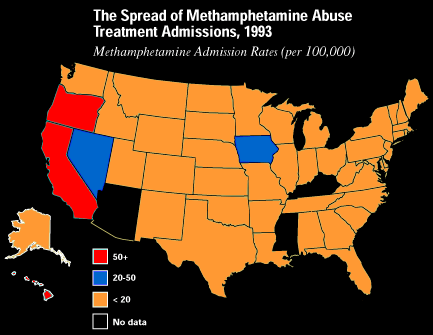
Overall usage. The 1997 NHSDA estimated that 5.3 million Americans (2.5 percent of the population) have tried methamphetamine in their lifetime, up significantly from the 1994 estimate of 1.8 million. The ADAM system reports that methamphetamine use continues to be more common in the western United States than in the rest of the nation. Methamphetamine use, according to ADAM, increased substantially in 1997, negating the progress achieved in 1996. In San Diego, roughly 40 percent of both male and female arrestees tested positive for methamphetamine.

Use among youth. The 1998 MTF survey asked 12th graders about the use of crystal methamphetamine known as "ice" -- which is smoked or burned in rock form. The survey found that lifetime ice use -- which had leveled-off at 4.4 percent in 1997 after a four-year rise -- rose in 1998 to 5.7 percent. The perceived harmfulness of methamphetamine among youth has also declined steadily since 1992 -- when 61.9 percent of 12th graders perceived "great risk" in trying "ice" once or twice -- to 1998, when only 52.7 percent perceived great risk.

Availability. Methamphetamine is by far the most prevalent synthetic controlled substance clandestinely manufactured in the United States. In the West and Southwest, it is increasingly significant as a drug of abuse: 52 percent of all those arrested in San Jose for drug possession, for example, test positive for methamphetamine. The Midwest has also seen an increase in methamphetamine production, trafficking and consequences. While the drug is not commonly found in the East and Southeast an analysis of methamphetamine treatment admissions as well as increased seizures suggest that the use of the drug maybe spreading eastward. The number of methamphetamine laboratory seizures reported to the Drug Enforcement Administration (DEA) in 1997 increased dramatically, to 1,431 from 879 in 1996. This reflects the widespread proliferation in the manufacture, trafficking, and use of the drug across the West and Midwest and portions of the South. During 1997 methamphetamine prices nationwide ranged from $3,500 to $30,000 per pound, $400 to $2,800 per ounce, and 37 dollars to $200 per gram.

Source:
SAMHSA, OAS, TEDS (Jan 1998)
The history of methadone and methadone prescribing
Responses to opiate use vary across the world and are, in many ways, as much a product of history as of anything else.
Understanding the history of responses to opiate use puts into context the prescribing policies we see today - and may help us anticipate the future.
Starting with the first organised responses to opiate use in the UK this section describes the influences on policy and practice, including those from the USA, the history of the discovery of methadone and the development of its unique role in the treatment of opiate use.
The services offering a treatment response to opiate use that are currently available in the UK are then described in the light of the historical background.
The origin of legal controls
At the turn of the century most countries had few laws restricting the possession of drugs.
Growing international concern about opiate use led to the First Opium Convention in the Hague in 1912. Britain as a signatory agreed to the principle of adopting controls over opium, morphine and cocaine.1
In July 1916, following rumours that soldiers on leave were using cocaine, a 'Defence of the Realm Regulation' was enacted making it illegal to possess cocaine unless prescribed by a doctor.
In 1920 and 1923 the list of drugs that were illegal to possess, import or sell was expanded by the Dangerous Drugs Acts to include opium and opium derivatives such as heroin. Doctors could still prescribe these drugs, but each prescription could only be for a maximum of three collections from the pharmacy.
This caused some concern among doctors because it left them unclear as to when prescribing these drugs was legitimate and was seen as Home Office interference with medical autonomy.
In 1924 the Ministry of Health set up a committee, chaired by Sir Humphrey Rolleston, to look into these issues.
The Rolleston report
This report, published in 1926, accepted the principle that all doctors could legitimately prescribe addictive drugs as part of the treatment of dependence. The report argued that abstinence should be the long-term goal of treatment, but also accepted that long-term prescribing was a legitimate way of treating people who were unable to stop taking drugs.
It recommended that two groups receive treatment with morphine or heroin, namely:
Those
who are undergoing treatment for the cure of addiction by the gradual withdrawal
method, and
Persons for whom, after every effort has been made for the cure
of the addiction, the drug cannot be withdrawn either because:
complete withdrawal
produces such serious symptoms which cannot be satisfactorily treated under the
normal conditions of private practice; or the patient, while capable of leading
a normal life so long as he takes a certain non-progressive quantity, usually
small, of the drug of addiction, ceases to be able to do so when the regular allowance
is withdrawn.
This pragmatic approach in which the care of opiate users was
entrusted to doctors continued without serious review until the late 1950s. However
the number of people being treated at any time was only a few hundred - and they
were generally considered to be stable.
When the first statistics were compiled in 1935 they counted 700 'addicts'. About one sixth of these were medical practitioners. This size and pattern of addiction remained similar through the 1930s, '40s and '50s. In 1959 there were 454 known addicts of whom the majority (204) were addicted to morphine, 68 to heroin and 60 to methadone. 76% had become addicted following treatment for pain and 15% were health professionals.2
The
discovery of methadone
The origins of the research
In 1939 Otto Eisleb and a colleague O Schaumann, scientists working for the large chemicals conglomerate I G Farbenindustrie at Hoechst-Am-Main, Germany, discovered an effective opioid analgesic drug which they numbered compound 8909 and called Dolantin.3 This was the discovery of pethidine. As with diamorphine (heroin) before, and buprenorphine (Temgesic) since, the early hopes of it being 'a new non-addictive analgesic' were not realised.
However the powerful analgesic action of pethidine was much needed during the Second World War. It was being produced commercially by 19393 and at the height of the war in 1944 annual production had risen to 1600 kg.4
Meanwhile close colleagues Max Bockm�hl and Gustav Ehrhart were working on compounds with a similar structure to Dolantin in the hope of finding:
- Water-soluble hypnotic (sleep-inducing) substances5
- Effective drugs to slow the gastrointestinal tract to make surgery easier6
- Effective analgesics that were structurally dissimilar to morphine - in the hope that they would be non-addictive5 and escape the strict controls on opiates.
There is no evidence, as had been widely believed both here and in the USA, that they were working as part of a German attempt, directed by Hitler, to replace opium supplies which had been cut off by the war.
This myth has been widely expanded to attributing one of methadone's first trade names - Dolophine - to being a derivation of Adolf and even that it was called Adolophine in Germany - the 'A' being dropped after the war. In fact the name Dolophine was created for the drug as a trade name after the war by the Eli-Lilly pharmaceutical company in America. It was probably derived from the French dolor (pain) and fin (end).6
The discovery of 'Hoechst 10820': methadone
During 1937 and the spring and summer of 1938 Bockm�hl and Ehrhart worked on the creation of another new substance in the group which they called 'Hoechst 10820' and, later, polamidon.
A patent application was filed on 11 September 1941 and the discovery was formally credited to Bockm�hl and Ehrhart (see overleaf).7
It
has been asserted that because the new compound's two-dimensional structure had
no resemblance to morphine its pain-killing properties were not recognised until
after the war had ended.6 But although the town of Hoechst was extensively bombed
during the war the I G Farbenindustrie factory suffered only slight damage and
so limited experimental work was able to continue, stopping only when supplies
of coal ran out or when the rail links were broken. In the autumn of 1942, after
it had been determined that the drug was both an analgesic and a spasmolytic,
it was handed over to the military for further testing under the code name Amidon.8
There was no attempt to try and get polamidon production levels up to those of
pethidine. Construction continued at Hoechst on a new pethidine production plant.4
An explanation for it not being exploited more fully between 1939 and 1945
was given by Dr K K Chen - an American doctor who did much of the early clinical
research work after the war - who said a former employee of I G Farbenindustrie
had told him in personal correspondence that they had discounted its use because
of the side effects.8 Chen presumed that the doses used in the experiments had
been too high, causing nausea, overdose etc.
After the war
All German patents and trade names, including those for polamidon, were requisitioned by the allies as spoils of war. The I G Farbenindustrie factory was in a US occupation zone and therefore came under American management. The US Foreign Economic Management Department sent a 'Technical Industrial Intelligence Committee' team of 4 men (Kleiderer, Rice, Conquest and Williams) to investigate the war-time work at Hoechst.
In 1945 The Kleiderer report was published by the US Department of Commerce Intelligence. For the first time in print it reported the findings of Bockm�hl and Ehrhart; and that despite having a different structure, polamidon closely mimicked the pharmacological action of morphine.9
The formula was distributed around the world and exploited by many companies, which is why it has so many different trade names. As a result this production of analgesics, which was no longer commercially viable, practically stopped at Hoechst after the war. The pethidine plant, by then half finished, was instead dedicated to the production of penicillin.4 The I G Farbenindustrie empire was broken up by the allies and the plant that had developed methadone became part of a new company called Hoechst A G.
Eli-Lilly and other American and UK pharmaceutical companies quickly began clinical trials and commercial production of the new drug, polamidon.
In 1947 Isbell et al, who had been experimenting extensively with methadone, published a review of their experimental work with humans and animals and clinical work with medical patients.10 They gave volunteers up to 200mg 4 times daily, and found rapidly developing tolerance and euphoria. They had to reduce levels with patients on these high doses because of, among other things: '...signs of toxicity ... inflammation of the skin ... deep narcosis and ... a general clinical appearance of illness.' They also found that 'morphine addicts responded very positively.' They concluded that methadone had high addiction potential: 'We believe that unless the manufacture and use of methadon [methadone] are controlled addiction to it will become a serious health problem.'
There were many early studies all of which found methadone to be an effective analgesic. Bockm�hl and Ehrhart were not able to submit the preliminary research results that they had given to Kleiderer on the 60 or so compounds they had discovered in the 'new class of spasmolytic and analgesic compounds' until July 1948. They were published in 1949.11
Early
use in the UK
The earliest accounts of methadone use in the UK were from papers published in the Lancet in 1947 describing it as 'at least as powerful as morphine, and 10 times more powerful than pethidine' and, subsequently, a study of its use as an obstetric analgesic at the University College, London.12 This study, however, was terminated because of respiratory depression in the newborn babies.
Early advertisements claimed that Physeptone (Wellcome's trade name for methadone) carried 'little risk of addiction' and the consensus was that it was a better analgesic than morphine. It is therefore likely that the first people who became dependent on it had either been treated for pain or treated by doctors who thought it to be less dependency-forming than other opiates.
In 1955 the Home Office was aware of 21 methadone addicts; by 1960 the number had risen to 60.2 In 1968 when the present Home Office notification system was set up the first two notifications arrived on 1 January: a 19 year-old female from London SW12 and a 20 year-old male from London SE23. By the end of the year 297 people had been notified as addicted to methadone.13 In 1969, as a result of the setting up of clinics (see below) the number of people reported as using methadone had risen to 1687.14
The 1960s
In 1958, at the instigation of the Home Office, the Department of Health set up a Committee on Drug Addiction to review policy in the light of the new synthetic opiates that had come on to the market. The report, often called the 'First Brain Report', was published in 1961. Its conclusions were, effectively, an endorsement of the Rolleston report.
In the early 1960s the number of opiate addicts increased and the pattern of use began to change: there were younger people and more people taking opiates for pleasure rather than as part of medical treatment.
Heroin first overtook morphine as the most notified drug of addiction in 1962.15 Most of these 'new' addicts lived in London. All of the heroin was pharmaceutically pure and much of it was prescribed by a small number of doctors.
There was concern that, contrary to the principles of the Rolleston report, some doctors were showing little, if any, inclination to 'make every effort for the cure of addiction'. This concern led to the recall of the Committee on Drug Addiction in 1964.
The second Brain report
This report was published in 1965 and resulted in changes in policy and the law:
- The right to prescribe heroin and other specified controlled drugs for the treatment of addiction was restricted to doctors licensed by the Home Office
- Doctors were legally required to notify addicts to the new Home Office Addicts Index
- Drug clinics were set up to provide specialised medical treatment of addiction.
Contrary to the belief of many doctors methadone has never been one of the controlled drugs that can only be prescribed by specially licensed doctors.
The late 1960s
By 1966 there were 6 times more notified heroin addicts than morphine addicts.15
In 1968 the new drug clinics began operating. Their establishment attracted a large population of opiate users into contact with the service and the number of notified addicts rose to 2881 of whom 2240 were addicted to heroin. The clinics were set up to:
- Provide a legal supply of drugs
- Attract heroin users into contact with the service
- Prevent the illicit market in drugs
- Prevent the crime associated with illicit drug use
- Help people get off drugs altogether.
In the first years of the drug clinics they prescribed drugs that the clients were already taking, mostly in injectable form. Some clinics had 'fixing rooms' where injecting equipment was provided so that clients could inject their medication.
By the end of 1969, in central London, diverted supplies of injectable methadone, mostly in the form of Physeptone ampoules and 10mg diamorphine tablets, were huge. These tablets were known as 'Jacks' which is the origin of the phrase 'Jacking up'. Indeed Physeptone ampoules were so easily available on the black market that they were used:
- As a suitable sterile fluid to flush out and clean injecting equipment between 'hits' of 10mg diamorphine tablets
- Instead of water to dissolve drugs
- As a 'freebie' to encourage bulk sales of the 10mg diamorphine tablets.
These supplies came from both the clinics and a small number of doctors in central London who had large numbers of opiate users on their lists to whom they prescribed freely.
The 1970s
During the 1970s the incidence of heroin use continued to rise. For the first time this included a significant quantity of imported, illicit heroin.
The clinics started to doubt the efficacy of prescribing the client's drug of choice as a way of producing change. Clinic prescribing practice moved away from predominantly prescribing injectable heroin towards prescribing oral methadone, on the basis that it was more therapeutic to prescribe a non-injectable drug and because its long half-life meant it could be taken once daily rather than every few hours.
A landmark study from that time (and the only randomised controlled trial in this area) compared the effects of randomly allocating heroin users to either of these two treatments.16 The study, carried out by Martin Mitcheson and Richard Hartnoll between 1971 and 1976, found that methadone treatment produced more polarised effects than heroin treatment. The methadone group were more likely to leave treatment but were also more likely to achieve abstinence. The heroin group were more likely to stay as they were. The researchers concluded that:
'The provision of heroin maintenance may be seen as maintaining the status quo, although ameliorating the problems of acquiring drugs ... by contrast the refusal to prescribe heroin (and offer oral methadone instead) may be seen as a more active policy of confrontation that is associated with greater change.'
As the results of this study became available the clinics were starting to deal with a new and different client group: large numbers of working-class heroin users who were smoking rather than injecting the relatively cheap heroin that had appeared on the market from the Middle East.
In the light of the changing client group - who were not asking for injectable drugs - and the results of the study, the clinics defined their role as one of promoting change and increasingly moved towards the use of oral methadone.
The shift away from maintenance prescribing
Some clinics began to review the efficacy of maintenance prescribing. For example a small study carried out in 1975 by the Glasgow Drug Clinic found that ceasing to prescribe methadone to new patients led to them improving as much as maintained patients, except in the area of crime.17 Although weak scientifically, the publication of studies such as this in the late 1970s led to questioning of the value of maintenance prescribing, or, indeed, any prescribing.
The 1980s
In the early 1980s there was a second period of dramatic increase in the prevalence of heroin use. The numbers of notified addicts which had increased slowly through the 1970s from 509 in 1973 to 607 in 1976 and to 1110 in 1979, doubled from 1979 to 1982 and had doubled again by 1984.18
This great increase in the early 1980s differed from that of 20 years earlier, in that it was not restricted to London: it occurred all over Britain and many of these new users smoked their heroin (known as 'chasing the dragon') rather than injecting it.
The prescribing response was largely one of methadone mixture detoxification programmes - the 'gradual withdrawal method' of the Rolleston report.
However the increase in the number of opiate users meant that services had to expand and become more widely available. Prompted by this change and the Advisory Council on the Misuse of Drugs (ACMD) Report on Treatment and Rehabilitation19 the Government responded with a funding initiative which saw the development of a non-statutory drug service and/or a Community Drug Team in most health districts. Most of these new services got involved in methadone prescribing either by employing a clinical assistant or a consultant psychiatrist on a sessional basis to prescribe methadone, or through working with GPs.
AIDS and the re-emergence of maintenance prescribing
The possibility of rapid transmission of the HIV virus among intravenous drug users and reports of high HIV prevalence figures among intravenous drug users in Edinburgh prompted a fundamental review of drugs policy.
The 1988 report of the Advisory Council on the Misuse of Drugs (ACMD) on AIDS and drug misuse20 Part 1 led to the development of community-based needle and syringe exchange schemes all over Britain.
The report articulated the policy of directing treatment towards abstinence by achieving intermediate goals such as:
- Stopping injecting with unsterile equipment
- Taking drugs by mouth or inhalation
- Taking prescribed rather than illegal drugs.
The report advocated a comprehensive approach to the prevention of the spread of HIV, following its first conclusion that:
'...HIV is a greater threat to public and individual health than drug misuse. The first goal of work with drug misusers must therefore be to prevent them acquiring or transmitting the virus. In some cases this will be achieved through abstinence. In others, abstinence will not be achievable for the time being and efforts will have to focus on risk reduction. Abstinence remains the ultimate goal but efforts to bring it about in individual cases must not jeopardise any reduction in HIV risk behaviour which has already been achieved.'
This reversed the abstinence-orientated prescribing policy of the preceding years as it legitimised longer-term prescribing to enable users to stop injecting. Although there was a wider range of prescribing options supplementing short-term detoxification, most doctors continued to prescribe methadone mixture only for limited periods of time.
In time it transpired that the high HIV infection rates in Edinburgh were a local phenomenon resulting from factors such as unavailability of injecting equipment, and were not being replicated across Britain.21, 22 However the services that were set up on the assumption that these HIV prevalence rates were typical have almost certainly been instrumental in maintaining relatively low rates of HIV seroprevelance among injecting drug users.
The opposition to methadone maintenance prescribing
This shift was not universal. The prescribing clinic in Sheffield was disbanded and replaced by short-term in-patient detoxification and residential rehabilitation.23 At first in Edinburgh - where the epidemic of HIV had left half of the city's injectors HIV positive - methadone was only offered to those who were HIV positive. It took until 1988 to establish a co-ordinated prescribing service.24
In Merseyside some doctors revived the prescribing of heroin in injectable and smokeable forms.
The 1980s conflict over prescribing policy led many to regard as a cause c�l�bre the disciplining of Dr Anne Dally who had espoused maintenance prescribing. The General Medical Council found Dr Dally guilty of 'serious professional misconduct' because she had 'irresponsibly treated addicts privately by providing methadone in the long term without reasonable medical care.' Some saw this as punishment by the medical establishment for her policy of maintenance prescribing and prescribing of injectables as part of private practice.25, 26
The American experience
It is helpful to understand the American experience with methadone maintenance because:
- This is where the concept originated
- Of the different ways in which treatment has been delivered there
- Much of the research into methadone treatment has been carried out in the USA.
The American experience shows that treating patients with the same medication can be viewed and executed in very different ways, and that these may be as important as the drug itself in determining the effects of treatment.
From the First World War onwards American and British drug policies took very different directions. In the USA in 1914 the Harrison Act controlled the sale and possession of drugs. It contained references to the prescription of addictive drugs for 'legitimate medical purposes ... prescribed in good faith'. However in 1922 the Behrman case, in stark contrast to UK policy, determined that it was a crime for a physician to prescribe a narcotic drug to an addict.
By 1938 approximately 25000 doctors had been prosecuted on narcotics charges and 3000 had served prison sentences! Federal agents relied heavily on the testimony of drug users to secure these convictions - they secured these testimonies by supplying the users with small quantities of drugs.6 Understandably this resulted in doctors having very little to do with the treatment of addiction.
After the Second World War there were just two large drug treatment facilities providing in-patient treatment to 'help addicts abandon drug taking'. The one at Fort Worth in Texas offered a service to men who lived west of the Mississippi and the one in Lexington in Kentucky served men east of the Mississippi and women from the entire USA.
The first use of methadone in the treatment of opiate dependence
An account of the first use of methadone in the treatment of addiction given by Dr M J Kreek in 1989 is quoted by Thomas Payte.6
In the early 1960s Dr Marie Nyswander and Dr Vincent Dole, a respected American psychiatrist and research scientist, had found that they could not stabilise opiate users on morphine without continually increasing the dose. They reviewed the medical literature in search of possible alternatives and pioneered the radical step of prescribing methadone which was effective orally, and seemed from pain research and some detoxification experience to be longer acting (they were not able to measure blood levels in those days). They soon found that once they had reached an adequate treatment dose that they could maintain people on that dose for long periods of time.
Dole encountered powerful resistance from the US Bureau of Narcotics whose agents told him that he was breaking the law and that they would 'put him out of business'. In view of the past history of doctors' experiences in court he took the brave step of inviting them to prosecute so that a 'proper ruling on the matter could be made' - they declined.
Nyswander and Dole: the pioneers of American methadone maintenance
Within a year Nyswander and Dole had developed 'Methadone Maintenance Treatment'. Their experiments with this approach began with treating people in a locked ward with elaborate security procedures. The project soon discovered that this level of security was unnecessary and it was gradually abandoned by moving first to an open ward, and then having patients reside in the ward whilst they went out in the daytime to work. This innovative treatment was offered only to people with a long history of heroin use and failed treatment.
Nyswander and Dole based their approach on the theory that, once addicted, opiate addicts suffer from a metabolic disorder, similar in principle to metabolic disorders such as diabetes. Just as insulin normalises the dysfunction in diabetes, so methadone was proposed to normalise the dysfunction of opiate addiction. They argued the necessity for large doses of methadone (80mg to 150mg) to establish a 'pharmacological blockade' against the effects of heroin, that would prevent addicts from experiencing euphoria if they took it.
Even though Nyswander and Dole viewed methadone treatment as a physical treatment for a physiological disorder, their initial attempts to use methadone maintenance were combined with intensive psycho-social rehabilitation. Many of their patients clearly derived great benefit from this innovative treatment.27
The spread of methadone maintenance programmes
This new form of treatment spread rapidly in the USA but was often implemented in a rigid way that lost some of the characteristics of Nyswander and Dole's original work. Consequently few programmes have produced such good results as their early work. The ways in which it was implemented in the early 1970s were strongly affected by political and other factors, with extensive government regulation.
The medical treatment was - and is - encased in a rigid delivery system. In most programmes patients attend the programme daily to drink their methadone and are regularly monitored through testing of urine samples (the collection of which is supervised) and counselling. Some programmes offer a variety of help and psycho-social treatment from group therapy to help in finding jobs. Once patients are stabilised they are able to earn the 'privilege' of taking home doses of methadone for one or more days.
The numbers of patients receiving Methadone Maintenance Treatment (MMT) in the USA rose: in 1992 there were about 120000 patients served by around 800 programmes. There is a great deal of variation in the rehabilitation and psycho-social services that are offered in addition to methadone and also in the dosage levels employed. Over half of patients receive below 60mg daily - which is accepted in the USA as the therapeutic minimum28 - well below the level recommended by Nyswander and Dole's research.
Prescribing services available in the UK today
Methadone prescribing services in the UK could be described as a patchwork, with most areas having a service of some kind but with many variations between health districts. The titles of services can vary a lot but, in addition to GPs, there are three main types of community service:
- Street agencies
- Community drug teams
- Drug clinics.
There are also a small number of doctors who offer treatment to drug users as part of:
- Private medical practice.
General Practitioners (GPs)
Everyone has the right to have a GP. Although many refuse to treat drug dependency all GPs are entitled to prescribe methadone (and most other drugs) in order to treat addiction. GPs notify nearly half of all those treated with methadone.
They do not usually have in-house testing facilities such as urinalysis, but primary health care teams increasingly have staff such as counsellors in their surgery.
GPs vary considerably in their attitudes and practice in treating drug problems. If a GP is not inclined to prescribe methadone for an opiate user there is little that can be done to force them because doctors are able to use considerable discretion in deciding what they think is the best treatment for their patients.
Street agencies: easy-reach, often non-statutory services
Such services are often called the 'Drug Advisory Service' or similar and tend to be based in town centres, designed to be easily accessible and easy to approach. They may be staffed by a mix of paid staff and voluntary workers, usually providing a telephone helpline, advice and counselling, needle exchange and guidance on how to access residential rehabilitation and detoxification or methadone treatment. They usually serve a wide range of people with drug problems, and their families.
Community drug teams (CDT)
Statutory services are usually staffed by nurses and social workers and in some cases also by clinical psychologists, probation officers, counsellors, and/or medical practitioners. Some community drug teams play the same role as street agencies, but usually focus on a prescribing and counselling service. They may have their own doctor to prescribe, or may liaise with the patient's GP to put together a package of care involving monitoring and counselling from the CDT. CDTs tend to serve mainly opiate users, but usually have a remit to help people and their relatives with other types of drug problems.
Drug clinics
Drug clinics tend to be based in hospital and emphasise out-patient medical care; they are often headed by a consultant psychiatrist, but staffed by doctors, nurses, social workers, and possibly occupational therapists and/or clinical psychologists.
Clients may have to attend on a daily basis or several times a week to obtain their prescriptions. In some cases, usually 'low threshold methadone maintenance programmes', they may be required to drink their methadone at the clinic in front of a member of staff.
To cope with the large volume of prescription writing most clinics use a computer to generate prescriptions - see Section 5: methadone and the law, handwriting exemptions. These prescriptions may then be sent to retail pharmacies for dispensing. Alternatively, methadone may be dispensed from a local hospital pharmacy as this is often cheaper.
Drug clinics may have access to specialist in-patient facilities for detoxification and other in-patient treatments. Some clinics have facilities for dispensing methadone to patients who have to attend daily to receive their medication. Drug clinics usually offer a variety of treatment options.
Large centre prescribing is often an essential part of a service to a large number of opiate users, hence their predominance in large cities.
Private practice
Despite the experience of Dr Anne Dally (see above) there are still a small number of doctors in private practice who prescribe oral or injectable methadone to drug users. Some do it out of a belief in the need for more sympathetic, responsive services and offer a useful adjunct to the NHS. Others are not so principled, and some of these are still a source of drugs for the illicit market, and are of little therapeutic value to their patients. However, large dose, unsupervised prescribing is not confined to private practice and is a feature of a minority of all service types.
In general, private services are preferred by clients who are in full-time employment, and appreciate the shorter waiting times, increased doses and willingness to prescribe on a maintenance basis.
Cocaine's
Role in American History
Cocaine was first synthesized in 1855. It was not
until 1880, however, that its effects were recognized by the medical world. The
first recognized authority and advocate for this drug was world famous psychologist,
Sigmund Freud. Early in his career, Freud broadly promoted cocaine as a safe and
useful tonic that could cure depression and sexual impotence. Cocaine got a further
boost in acceptability when in 1886 John Pemberton included cocaine as the main
ingredient in his new soft drink, Coca Cola. It was cocaine's euphoric and energizing
effects on the consumer that was mostly responsible for skyrocketing Coca Cola
into its place as the most popular soft drink in history.
From the 1850's to the early 1900's, cocaine and opium laced elixirs, tonics and wines were broadly used by people of all social classes. This is a fact that is for the most part hidden in American history. The truth is that at this time there was a large drug culture affecting a broad sector of American society. Other famous people that promoted the "miraculous" effects of cocaine elixirs were Thomas Edison and actress Sarah Bernhart. Because there were no restrictions placed on acquiring these drugs in the early 1900's, narcotics were an acceptable way of life for a large number of people, many of whom were people of stature. Cocaine was a main stay in the silent film industry. The pro-drug messages coming out of Hollywood at this time were receiving international attention which influenced the attitudes of millions of people about cocaine.
As a rule, famous people are role models that can and do influence the masses. Star power has proven time and again to be the most potent form of advertising. Think about it: The worlds most famous psychologist; the man that invented the light bulb; a stable of Hollywood silent film stars; and the inventor or the most popular soft drink in history - all on the pro-cocaine band wagon. All promoting the drug's positive effects. Some did it through personal testimonials that ran in printed pages across the nation. Others (in particular the silent film stars) promoted cocaine's acceptability through the examples they set by their well publicized life styles.
In the same way as other narcotics like opium and heroin during this time, cocaine also began to be used as an active ingredient in a variety of "cure all" tonics and beverages. In many of the tonics that drug companies were producing at this time, cocaine would be mixed with opiates and administered freely to old and young alike. It wasn't until some years later that the dangers of these drugs became apparent.
In fact, it was the negative side effects of habitual cocaine use that was responsible for coining the phrase, "dope fiend". This terminology came about because of the behavior of a person abusing cocaine for prolonged periods of time. Because cocaine is such a powerful stimulant, prolonged daily use of the drug creates severe sleep deprivation and loss of appetite. A person might go days or sometimes weeks without sleeping or eating properly. The user often experiences psychotic behavior. They hallucinate and become delusionary. Coming down from the drug causes a severe state of depression for the person in withdrawal. This person can then become so desperate for more of the drug that they will do just about anything to get more of it, including murder. If the drug is not readily available, the depression one experiences in withdrawal can become so great the user will sometimes become suicidal. It is because of this heinous effect on the user that the word "fiend" became associated with cocaine addiction.
Over the course of the next several years the American majority became more and more aware of the dangers of cocaine. As the severity of this problem became more and more apparent, concern mounted to an eventual public outcry to ban the social use of cocaine. This public pressure forced Pemberton to remove cocaine from Coca Cola in 1903. Eventually the public pressure became so great as to place a national prohibition on cocaine. The country's legislators took notice, and in 1920 cocaine was added to the list of narcotics to be outlawed by the passing of The Dangerous Drug Act of 1920. Unfortunately, as with the opiates like heroin, the dangers of cocaine abuse were recognized by law makers after the fact. The market for cocaine had already been established and was deeply entrenched into American history and culture and is with us today.
History
of Cocaine Timeline
courtesy erowid.org
| c. 3000 B.C. | Coca chewing is practiced throughout South America. Coca is believed to be a gift from God. |
| 1400s | Coca plantations are operated by Incas in Peru. |
| 1505 | First hand accounts of coca use made their way back to Europe. Amerigo Vespucci (1505), G Frenandez de Oviedo (1535), and Nicholas Monardes (1565). |
| Early 1500s | Incan Coca plantations are taken over by holders of Spanish land grants. Spanish tax laws are revised to allow land owners to make their tax payments in coca leaves. |
| 1539 | The Bishop of Cuzco tithes coca, taking 1/10 of the value of each crop in taxes. |
| Mid 1500s | Coca production in Peru expands quickly causing a glut of leaf on the market which in turn precipitated a drop in the price of coca. |
| 1574 | Monardes' text on Coca is first translated into other European languages from Spanish; Latin (1574), Italian (1576), English (1577). |
| 1575 | Forced laborors working in the Spanish silver mines were kept well supplied with Coca leaves. Roughly 8\\% of the Europeans living in Peru were involved in the Coca trade. |
| 1662 | Abraham Cowley writes a poem titled "A Legend of Coca". This is the first independent mention of coca in English literature. |
| 1708 | Coca is first mentioned in a materia medica, Institutiones Medicae, written by German physician and botanist Herman Boerhaave. |
| 1835 | First accurate drawing of Coca appears in popular English press. The illustration by Sir William Hooker, director of the Kew gardens, was published in Companion to the Botanical Magazine. |
| 1850 | Coca tinctures used in throat surgery. |
| 1855 | Cocaine first extracted from Coca leaves. |
| 1862 | Merck produces 1/4 pound of cocaine. |
| 1869 | Seeds from the commercial variety of Coca arrived at Kew Gardens. |
| 1870 | Vin Mariani (Coca wine) is for sale throughout France, containing 6 mg cocaine per ounce of wine. Exported Vin Mariani contained 7.2 mg per ounce to compete with the higher cocaine content of American competitors. |
| 1870s | Parke,Davis manufactures a fluid extract of coca. |
| 1876 - 1885 | Race walkers in England chew Coca leaves to improve their performance. |
| 1883 | Merck produces 3/4 pound of Cocaine. |
| 1884 | Cocaine's use as a local anesthetic in eye surgery is popularized. |
| 1884 | Freud publishes On Coca in which he recommends the use of cocaine to treat a variety of conditions including morphine addiction. |
| 1884 | Merck produces 3,179 pounds of Cocaine. |
| 1886 | Merck produces 158,352 pounds of Cocaine. |
| 1886 | Coca-Cola is first introduced by John Pemberton, containing cocaine laced syrup and caffeine. |
| Late 1880s | Parke,Davis starts to manufacture refined cocaine. |
| 1901 | Coca-Cola removed Coca from their formula. |
| 1905 | Snorting cocaine becomes popular. |
| 1910 | First
cases of nasal damage from Cocaine snorting are written of in medical literature.
First cases of nasal damage from Cocaine snorting are seen in hospitals. |
| 1912 | U.S. Government reports 5,000 Cocaine related fatalities in one year. |
| 1914 | Cocaine banned in United States. |
| Early 1930s | Japan is the world's leading cocaine producer (23.3\%) followed by the United States (21.3\%), Germany (15\%), UK (9.9\%), France (8.3\%). |
| 1976 | Freebase cocaine first developed (probably in California). It would soon be popularized by dealers and glamorized by Hollywood media. |
| 1981 | Wholesale cost of 1 kg of cocaine is $55,000. |
| 1984 | Wholesale cost of 1 kg cocaine is $25,000. |
| Mid 1980's | Freebase cocaine becomes popular. |
| References
1
. The Encyclopedia of Psychoactive Drugs: Cocaine, A New Epidemic, by Chris- Ellyn
Johanson. | |
| Quote |

 |
| Link
to Us! |
Show your support, link to us! |
 Funding pledged to fight drug abuse
Funding pledged to fight drug abuse